Access to self-managed abortion is not a uniform experience
Women in India are increasingly turning to self-managed abortions.
It reflects a demand for care that is convenient and private.
But it also highlights gaps within India’s healthcare system.
This surging trend is meticulously documented in a study published in Global Public Health (2025).
By examining the experiences of over 700,000 women, the research reveals a landscape where the home has become the primary site of care for nearly half of all abortions in the country.
This evolution challenges long-standing social taboos and legal frameworks, signalling a future where reproductive agency is defined more by personal choice than by clinical gatekeeping.
The Surge of Home-based Care
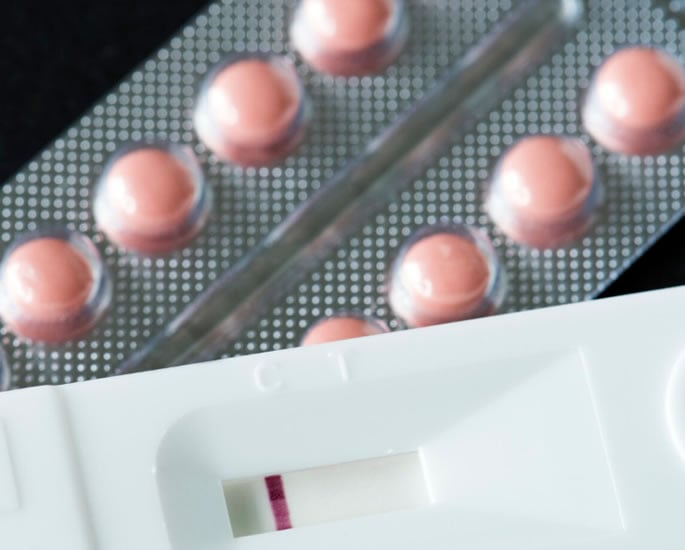
The shift toward self-managed abortion (SMA) in India is best understood through the lens of a massive eight-year data set that tracks a definitive move away from hospital-based procedures.
According to the analysis, the prevalence of SMA has more than doubled in a remarkably short period, reflecting a seismic change in health-seeking behaviour.
In 2014, self-managed abortions accounted for approximately 19% of all reported cases. By 2021, that figure escalated to 45%, representing a near-total transformation of the abortion landscape.
This surge corresponds with a significant decline in provider-assisted abortions, which dropped from 81% to 55% in the same timeframe.
This transition is fuelled by the increased availability and social acceptance of Medical Abortion (MA) pills, specifically the combination of mifepristone and misoprostol.
While the Medical Termination of Pregnancy (MTP) Act technically requires a prescription from a registered medical practitioner, the reality on the ground is far more fluid.
Widespread over-the-counter access at local pharmacies has allowed women to navigate their reproductive needs without the often-intimidating or judgmental clinical atmosphere.
The research defines SMA as an attempt to terminate a pregnancy using medical abortion performed outside of health facilities without clinical supervision.
For a growing number of Indian women, “clinical supervision” is increasingly viewed as a barrier they are willing to forego in favour of the immediate privacy offered by their own living rooms.
The numbers suggest that the home is no longer just a fallback option; it is becoming the preferred site of care.
This is particularly evident in states like Odisha, where the proportion of self-managed abortions has reached parity with provider-assisted care.
The trend is remarkably consistent across the eight-year study period, suggesting that this is not a temporary fluctuation caused by external events like the pandemic, but a permanent recalibration of how women interact with the healthcare system.
As self-management approaches the 50% mark, it is clear that the pharmacy and the home are superseding the clinic as the primary pillars of abortion access in India.
Divides in Reproductive Access

Access to self-managed abortion is not a uniform experience across the Indian subcontinent; instead, it follows distinct regional and socioeconomic fault lines.
The study reveals significant geographical disparities, with the highest proportions of SMA concentrated in the eastern (45%), central (39%), and north-eastern (31%) regions.
In sharp contrast, the southern and western regions report much lower rates, at 9% and 11% respectively.
These figures highlight a complex interplay between local healthcare infrastructure, regional cultural norms, and the physical density of retail pharmacies.
Socioeconomic status plays a pivotal role in determining who chooses, or is forced, to self-manage.
The multivariate analysis in the study indicates that women from economically disadvantaged backgrounds and those with lower levels of education have higher odds of opting for SMA.
Specifically, women with higher education had significantly lower odds (OR: 0.75) of choosing SMA compared to those with no formal education.
Employment status also emerged as a significant factor, with working women being 1.2 times more likely to opt for self-management than their non-working counterparts.
This suggests that for those with busy work schedules or limited financial resources, the speed and affordability of SMA are major draws.
The “why” behind these numbers often comes down to the logistics of survival.
For a woman in a rural village in Bihar or Chhattisgarh, the journey to a private clinic or a public hospital can involve expensive travel, lost wages, and the risk of being seen by community members.
The local pharmacy, however, is often within walking distance and offers a transaction that is over in minutes.
Interestingly, while rural women showed higher raw odds of opting for SMA than urban women, the study noted that this variation was not statistically significant once other wealth factors were controlled.
This implies that the drive toward self-management transcends the simple rural-urban divide and is more closely tied to specific regional cultures of self-reliance and the retail availability of medication.
Complication Rates and Clinical Realities

One of the most persistent arguments against self-managed abortion is the fear of medical risk, yet the data challenge the long-held assumption that “self-managed” equates to “high-risk”.
The study found that 12.6% of women who self-managed reported complications, which is actually lower than the 14.9% reported by those who underwent provider-assisted medical abortions.
When the researchers adjusted for various socio-demographic variables, they concluded that self-managed abortion was not associated with higher odds of complications compared to medical abortions performed by a clinician (OR: 0.83).
The data highlights that the primary factor determining the safety of an abortion is not the presence of a doctor, but the timing of the intervention.
Gestational age is the most significant predictor of health outcomes in the study.
Women who self-managed at less than two months of gestation had significantly lower odds of reporting complications than those who sought provider-assisted care at the same stage (OR: 0.7).
Complications for both self-managed and provider-assisted methods increased substantially once the pregnancy passed the three-month mark, where medical abortion is generally less effective and surgical intervention becomes more common.
These findings suggest that for early-term pregnancies, the safety profile of self-managing with MA pills is robust and reliable.
It aligns with 2022 World Health Organisation guidelines, which moved toward de-medicalising abortion care.
The data underscores that when women have access to the correct drugs and basic information, they are capable of managing the process effectively on their own.
The risk arises not from the lack of a clinician’s presence during the process, but from a lack of access to drugs during the later stages of pregnancy.
By separating the “act” of abortion from the “facility” of the clinic, this research reframes SMA as a safe, evidence-based health practice rather than a dangerous or desperate last resort.
Over-the-Counter Reality
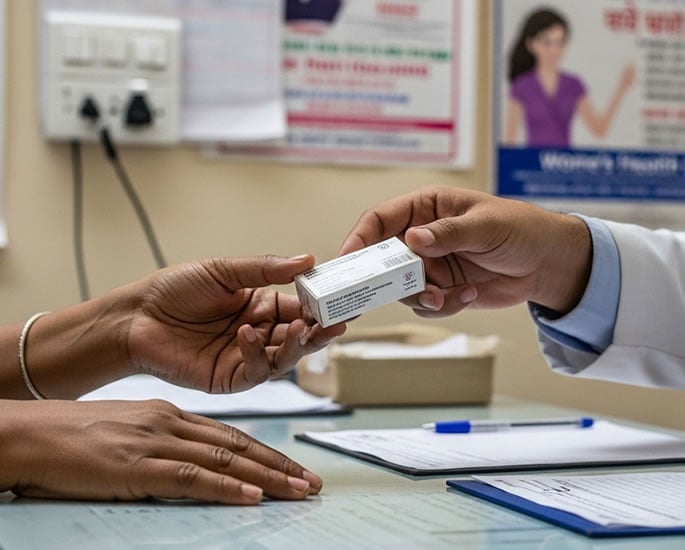
The legal framework for abortion in India exists in a state of constant tension with the actual practices of the population.
The original 1971 MTP Act was a progressive piece of legislation for its time, but it was deeply rooted in medical paternalism, viewing the physician as the ultimate gatekeeper of a woman’s body.
Even with the 2021 amendment, which extended the legal limit for abortion to 24 weeks for specific categories, the law remains clinician-centric.
However, the data reveals a massive “shadow market” that has effectively legalised abortion on the street level.
Pharmacy access is the engine driving this surge in self-management.
Despite the technical requirement for a doctor’s prescription to buy MA pills, they are widely available across India as a retail commodity.
This creates a fascinating paradox where a practice can be “legally restricted” but “functionally accessible” for anyone with a few hundred rupees.
The study notes that an estimated 73% of induced abortions in India, roughly 11.2 million cases every year, occur outside the formal health system.
This massive disconnect suggests that the formal healthcare system is failing to meet the demand for private, accessible care, leading women to build their own informal networks of support.
The role of the retail pharmacist has consequently become one of the most important pillars of Indian reproductive health.
For many women, the pharmacist is the only “provider” they will ever interact with, serving as a source of both the medication and the instructions for its use.
While this retail-led model offers a path to autonomy, it also places a heavy burden on the quality of information provided at the point of sale.
The rise of SMA is therefore a story of the deregulation of healthcare by the people themselves.
It reflects a growing movement to “depathologise” abortion, treating it not as a major medical crisis requiring hospital admission, but as a manageable health need that can be handled with the same privacy and dignity as any other personal matter.
The evidence presented by the data makes it clear that self-managed abortion is no longer a peripheral or “underground” phenomenon; it is a central feature of modern Indian life.
The dramatic shift from 19% to 45% in less than a decade signals a major change in how women perceive their reproductive options and exercise their agency.
By choosing the home over the clinic, women are successfully navigating around barriers of cost, travel, and social stigma, opting for a method that the data proves to be safe and effective for early gestations.
While regional and economic disparities continue to shape who can access this care, the overall trajectory points toward a future of increasing autonomy.
As the “transformative terrain” of Indian healthcare continues to shift, the reliance on self-management highlights a growing demand for privacy and the power of individual choice in the most personal of circumstances.






























































