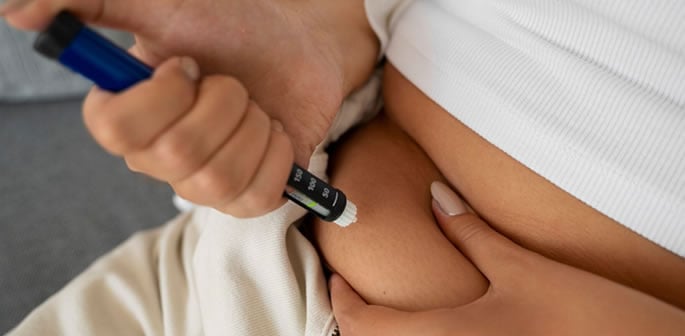
“The evidence from the clinical trial is compelling."
Weight-loss injections will be offered for free on the NHS to more than a million people in England at risk of heart attacks and strokes.
Also known as semaglutide, the drug will be offered to people at risk of heart attacks and strokes, even if they are not classified as obese.
Guidance from the National Institute for Health and Care Excellence (NICE) recommends the weekly jab for patients with a body mass index of 27 or above who have previously experienced cardiovascular issues.
This includes heart attacks, strokes or serious circulation problems in the legs.
Clinical trials involving tens of thousands of patients found semaglutide reduced the risk of heart attacks and strokes by around 20%.
Crucially, benefits were observed early, before significant weight loss occurred.
This suggests the drug works directly on the heart and blood vessels, not just by reducing body weight.
Each year, around 100,000 people in the UK are admitted to hospital with heart attacks, while another 100,000 experience strokes.
Approximately 350,000 people are living with peripheral arterial disease.
Experts estimate that up to seven in 10 cases of cardiovascular disease could be prevented.
Patients who have already suffered one event face a significantly higher risk of another, making early intervention critical.
Semaglutide will be offered alongside existing treatments such as statins and supported by lifestyle changes including diet and exercise.
Helen Knight, from NICE, said: “We know that people who have already had a heart attack or stroke are living with real fear that it could happen again.
“The evidence from the clinical trial is compelling. It showed that people taking semaglutide alongside their existing heart medicines were significantly less likely to have another heart attack or stroke.
“Today’s decision gives thousands of people in that situation an extra layer of protection, on top of the medicines they are already taking.”
Professor Robert Storey, a heart health expert at the University of Sheffield, warned GLP-1 drugs could reduce muscle mass as well as fat.
He said: “Physical activity, such as resistance training, is important to counteract potential negative effects on muscle strength.”
The Impact on British South Asians
Cardiovascular disease continues to disproportionately affect British South Asian communities, with earlier onset and higher complication rates widely documented across the UK.
A combination of genetic predisposition, higher rates of type 2 diabetes and increased central obesity contributes to this elevated risk profile, while dietary patterns that include refined carbohydrates and saturated fats can further increase risk.
Structural barriers also play a role, with delayed diagnosis often linked to gaps in culturally tailored healthcare, language barriers and limited targeted awareness campaigns.
For many, stigma around weight, illness and lifestyle changes continues to shape how and when people seek medical support.
The NHS rollout of semaglutide presents an opportunity to address these disparities through earlier intervention, particularly for those already at risk of cardiovascular events.
Welcoming the decision, Dr Sonya Babu-Narayan from the British Heart Foundation said she hoped the injections could be made available to everyone who could benefit “as soon as possible”.
Professor Naveed Sattar added: “This is very good news and stems directly from high-quality trial evidence.
“We now have medicines that not only reduce heart attacks, strokes and peripheral arterial disease but also simultaneously lead to meaningful weight loss, which in turn lowers the risk of many weight-related conditions.
“These treatments also improve patients’ quality of life in a meaningful way, making this a genuine win-win.”
By reducing the likelihood of repeat incidents, the treatment could help ease the long-term burden on communities that are statistically more vulnerable.
However, improving outcomes will depend on more than access alone, with culturally relevant outreach and clearer communication needed to ensure uptake is not limited.
How the Injections Help Reduce Risk
Semaglutide mimics the GLP-1 hormone, helping regulate appetite and slow digestion so patients feel fuller for longer and consume fewer calories.
This supports sustained weight loss, which reduces strain on the heart and improves key markers such as blood pressure and cholesterol levels.
Importantly, clinical evidence shows the drug also works directly on the cardiovascular system, with reductions in heart attack and stroke risk observed before significant weight loss occurs.
When combined with existing treatments such as statins, this creates a layered prevention strategy that strengthens overall protection.
For high-risk groups, including many British South Asians, this dual effect offers a more effective way to manage long-term cardiovascular risk.
What Happens Next
The rollout of semaglutide is expected to begin this summer, with NHS England indicating that eligible patients could access the treatment within months.
Around 1.2 million people are likely to qualify under updated guidance from NICE, marking a significant expansion of preventative cardiovascular care.
The NHS has reached an agreement with Novo Nordisk to ensure the treatment remains cost-effective at scale.
However, questions remain over whether services can meet demand, particularly as patients will require monitoring alongside prescriptions.
Treatment is currently capped at two years, and while long-term risks are still being studied, some experts believe extended use may be necessary to prevent relapse.
Despite these challenges, the shift towards preventative medicine is clear, with semaglutide positioned as a key tool in reducing cardiovascular disease before it escalates.